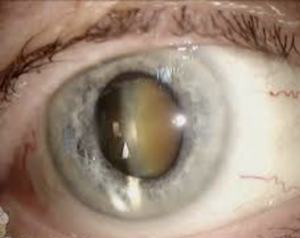
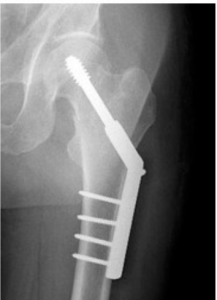
It would seem obvious that better vision results in fewer falls and therefore fewer fractured hips. Now a new study of more than a million US Medicare patients from Dr Victoria Tseng and colleagues, from the Medical School at Brown University, found that patients who had had cataract surgery were 16-28% less likely to break a hip in the year after the surgery compared to those who had not undergone surgery.
https://jamanetwork.com/journals/jama/fullarticle/1273017
Why are hip fractures a concern? A large study of elderly women found that within the subsequent 12 months of a fractured hip, the patient was twice as like to die compared to uninjured patients.
If you have been diagnosed with cataracts, or are having falls contact us on 93875300 to book an appointment with Dr Sharma in Bondi Junction or Miranda.
Find out if you are suitable for vision correction
Not everyone is eligible for vision correction surgery.
Find out if you could benefit from this life changing surgery by taking the quick self-suitability quiz below: